Pulmonary Embolism
A pulmonary embolism is a blood clot in the arteries of the lung. This blood clot causes harm in two ways. It prevents blood from picking up oxygen to deliver to the body. And, it elevates pressure in the lungs so that the right side of the heart cannot work properly.
Causes
Blood clots in the lung almost always come from blood clots in legs. Basically, a piece of a deep vein thrombosis that forms in the legs or in the pelvis breaks off and travels through the heart to the lungs.
There are three factors that contribute to blood clots:
- Blood not moving
- A tendency to clot. This is also known as hypercoagulability.
- Injury of the vein wall
We call these factors “Wirchow’s triad”. Sometimes we can identify the exact cause of the clot. When we can, we call the clot “provoked”. For example, a clot after surgery. Of course cancer and blood clots are a known combination. But many times we cannot find the cause. In these cases we call the clot “unprovoked”.
Symptoms
Not all blood clots will cause symptoms. In fact about a third of people who have clots in the lungs do not experience symptoms at all.
Still, pulmonary embolism symptoms do exist in most people with a pulmonary embolism. The most common symptoms will be:
- Chest pain
- Shortness of breath
- Rapid heart rate
The most severe symptoms will include:
- A drop in blood pressure. This happens when the pressure in the lung arteries is so high that the heart cannot push blood efficiently through the lungs.
- Syncope. This means loss of consciousness.
Diagnosis
We diagnose clots in the lungs with imaging studies. The most common way to make the diagnosis is with a CT scan. Here is an example of a CT scan showing blood clots in the arteries of both lungs:
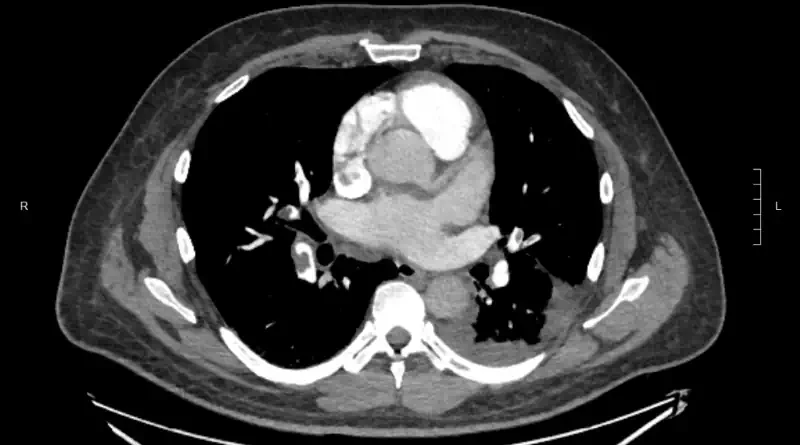
A CT scan involves radiation and contrast dye. So not every patient can have this test. Another test to diagnose pulmonary embolism is called ventilation / perfusion scan (V/Q scan).
How Severe is this Clot?
We divide pulmonary emboli according to their severity. This means that some clots are associated with a higher risk for the patient than others.
A lower risk clot might cause symptoms but is not putting a patient at risk. The heart is still working properly, and the patient is able to get oxygen into their bloodstream.
On the other hand, a high-risk clot put the patient at immediate risk. Either there is a risk for dying or there is a risk for low oxygen levels in the blood.
Intermediate-Risk Pulmonary Embolism
Finally, there are intermediate-risk blots. These are not low risk, but they are also not entirely high-risk. They may lead to poor outcomes. But often people improve with simple treatment with blood thinners. We define intermediate-risk pulmonary embolism according to the effect the clot has on the heart. On the one hand, there is no blood pressure drop. So, this is not the highest risk scenario. But on the other hand, we know how to identify some negative effects on the heart. For instance, blood testing might show that the heart is straining or injured. Or a heart ultrasound (echocardiogram) will show the right side of the heart enlarged or struggling to pump blood into the lungs. If a patient has an intermediate-risk pulmonary embolism, we need to observe them closely. We should try to identify patients who are deteriorating. If we notice signs of deterioration, we should consider treatments that are more aggressive than blood thinners. Unfortunately, it is often very hard to identify which patient will do well, and who will require more help.
Pulmonary Embolism Treatment
The most important treatment of a pulmonary embolism are blood thinners. It is important to start treatment as soon as possible. Delaying treatment means worse outcomes. In fact, more people will die if they receive treatment late.
If a person is short of breath, we should consider oxygen. This is especially true if we measure low blood oxygen levels.
We must make every effort not to miss the sickest pulmonary embolism patients. If a pulmonary embolism is severe enough to reduce blood pressure, we must assume that the patient has a very high chance of dying. For these patients, we need to consider aggressive treatments. The first treatment to consider are “clot busting” medicines. Another name for these medications is thrombolytics. Sometimes we will also consider procedures.
Procedures for Pulmonary Embolism
Sometimes we need to perform procedures for people with pulmonary embolism. First, if a patient is very sick, we need to consider connecting them to a machine that will support their circulation. This machine is called ECMO. Sometimes we will also need to support breathing. In these cases we will need to connect patients to a machine that will help them breath.
Sometimes we perform procedures to remove blood clots from the lung arteries. There are two types of procedures to do this:
- Lysis. This means dripping clot busting medications into the clot to help it dissolve quickly.
- Thrombectomy. This means sucking out the clot.
It is not always easy to know who to offer these procedures to. Of course, a patient who is very short of breath or whose heart is failing should have some form of aggressive treatment. But are there other pulmonary embolism patients who might benefit from a procedure? That is not an easy question to answer.


Pingback: Deep Vein Thrombosis: Symptoms, Diagnosis and Treatment
Pingback: Academic Medicine: How It Makes Me a Better Doctor Every Day
Pingback: Pulmonary Embolism Symptoms Can be Minor or Significant