Varicose Veins and Thrombosis
Varicose veins are enlarged, twisted veins that are commonly found in the legs. In some cases, blood flows more slowly in varicose veins than in normal veins. We know from Wirchow’s triad that blood that does not flow tends to clot. So, in theory, varicose veins and thrombosis will go hand in hand.
Epidemiology of Varicose Veins and Thrombosis
Varicose veins are associated with an increase in the risk of thrombosis. The relative risk for deep vein thrombosis is probably up to 5 fold compared to patients without varicose veins. If true, this is an impressive relative risk, on par with most conditions we can identify with sophisticated thrombophilia testing. Still, the absolute risk is still low. Furthermore, some studies have shown that varicose veins are an independent risk for clots, but not the only independent risk. For instance, recent hospitalization and older age also remain pertinent risk factors. Also, not all varicose veins are made the same. It is hard to imagine that one localized varicose vein poses the same risk as extensive varicose veins. There are no high quality data to help guide us there.
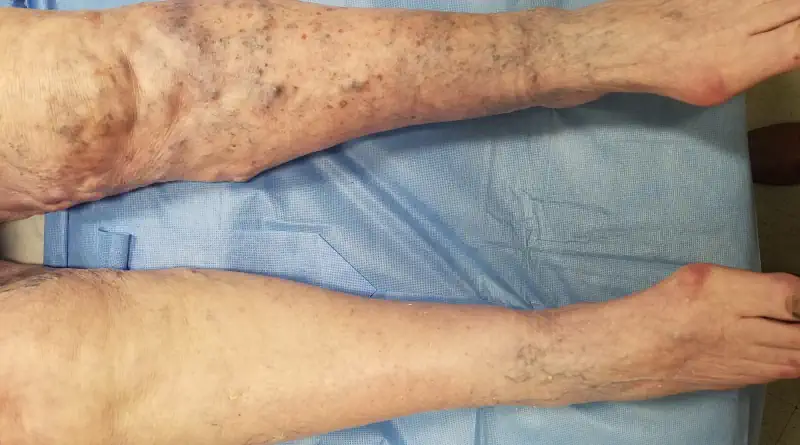
So, does the connection between varicose veins and increased risk for deep vein thrombosis mean there is benefit to treating varicose veins to prevent DVT? Not so fast… The data are not showing that.
Still, the risk for superficial thrombophlebitis is probably higher. In fact, they are one of the overlooked causes of blood clots in legs.
Superficial Vein Thrombosis Treatment
Obviously, not all superficial vein thrombosis arise from varicose veins. But I still think it makes sense to discuss their treatment here, because venous stasis and venous trauma are the most common causes. Decisions surrounding superficial vein thrombosis treatment revolve around three key factors:
- Clot location
- Extent of the clot
- Patient symptoms
Anticoagulation
In general, we will feel more compelled to offer anticoagulation for clots that are close to the deep system, extensive and associated with symptoms. When we offer anticoagulation, we typically treat for 45 days. But if the cause for the clot was not venous stasis, we should think about extending therapy (because it may signify more than “just” an anatomical issue). On the other hand, we will avoid blood thinners for clots that are localized, perhaps in a peripheral branch or varicose vein and with few symptoms.
When we do decide to offer anticoagulation, the two medications that were tested specifically are fondaparinux and rivaroxaban.
The first study to think about is CALISTO. Researchers randomized over 3000 patients to receive either fondaparinux 2.5 mg once a day or placebo for 45 days. They followed a combination of outcomes including death, pulmonary embolism and recurrent clot. Over the course of the study the outcomes occurred in 0.9% of the fondaparinux group but in 5.9% of the placebo group. On the other hand, major bleeding occurred in one patient in each group. Thus, at the end of the study they concluded that treatment was effective and with few side effects.
The second study is the SURPRISE trial. This time, 472 patients received either fondaparinux 2.5 mg or rivaroxaban 10 mg once a day. The study met the criteria of non-inferiority. I think the study population is interesting to note. It included patients with either extensive clots, or with other risk factors for clotting such as cancer or autoimmune disease. Specifically, the study did not include patients with varicose vein related clots.
Treating Varicose Veins and Thrombosis without Anticoagulation
Sometimes, we will not offer anticoagulation. But we still might want to help with symptom relief. In these cases, we can offer the following:
- Non-steroidal anti-inflammatory medications
- Warm compresses
Of course, in these instances, we need to make sure that the clot is not progressing. So, we need to follow the patient clinically. Also, we will sometimes repeat a scan within a few weeks of the diagnosis. That way, if we need to change our approach, we can try to catch the clot before it progresses into the deep system.
As a side note, any time we say “no anticoagulation” in the context of blood clots, one might think of IVC filters. But, none of the guidelines recommend IVC filters for superficial vein thrombosis. Therefore, we avoid them in this situation.
Treating Varicose Veins *AFTER* Thrombosis
Imagine a patient has a blood clot that is probably related to venous stasis. Let’s say you decided to treat with anticoagulation. Now, three months later, the patient asks you if a procedure to eliminate the refluxing incompetent vein makes sense. Well, I think it does make sense. And indeed, ablation and other procedures are common for the indication of preventing recurrent clot. But, the evidence to support this practice is not there. You can read a bit more about it in the European Society for Vascular Surgery 2021 Guidelines (scroll down to 2.11.6 and figure 11).




Pingback: Thrombophilia Testing: What is it? Should we test?
Pingback: Clot Recurrence: 11 Risk Factors to Consider in Each Patient
Pingback: Superficial Thrombophlebitis: Definition, Causes and Treatment